Stelara Formulary Update for April 1 2025
Stelara Formulary Change Effective April 1
Effective April 1, 2025, Stelara will no longer be a preferred drug on the Sanford Health Plan (SHP) formulary; instead, a biosimilar therapy- Wezlana- will be added as the preferred option.
Stelara will remain on the formulary, but with a brand penalty. A brand penalty is the price difference between a brand-name drug and the generic or biosimilar alternative; members pay this amount in addition to benefit plan cost-share. Brand penalties do not apply to the member’s deductible or maximum out-of-pocket costs.
Exceptions will be made on a case-by-case basis for members who have specific medical contradictions and certain circumstances that require them to stay on Stelara. Providers have been advised to begin the prior authorization process for members in this situation.
The grid below indicates how each medication will be positioned on the formulary; these updates will be reflected on the Sanford Health Plan website in April.
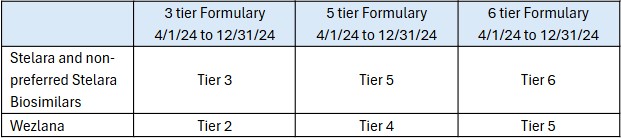
This change will affect less than 0.5% of our entire member population. A letter notifying those impacted was sent out this week. You can review a copy HERE along with the biosimilar fact sheet from the FDA. Providers have also been informed and will work with our members through the transition.
Sanford Health Plan will continue to implement these changes as more biosimilars continue to come to market. Many carriers are hoping for an organic shift to biosimilars, but we want to encourage the shift to capture savings on the costliest medication, both here at SHP and nationwide, as part of our continued commitment to being good stewards of our client and member premium dollars.
Please reach out to your account executive with questions. Thank you for your continued partnership.
